Working to improve care frequently requires working with complexity. This increases the challenge when trying to enable the spread and adoption of innovation, meaning we need a different way of leading and working.
Claire Roche (Director of Quality & Nursing, Welsh Ambulance Service Trust) joined Ian Baines (NHS Horizons, #ProjectA), in this video. In the video Claire shares her experience of developing and enabling the spread and adoption of the Welsh Ambulance Services Trust (WAST) falls framework, particularly reflecting on the seven spread principles and model of system convening.
The WAST falls framework was developed due to patient safety and patient experience concerns with people who had fallen and waiting quite a long time for help to arrive. In particular, the waiting times and potential subsequent harm to those who fell and were not injured so not initially a very high priority.

The Falls Framework and the 7 Spread and Adoption Principles
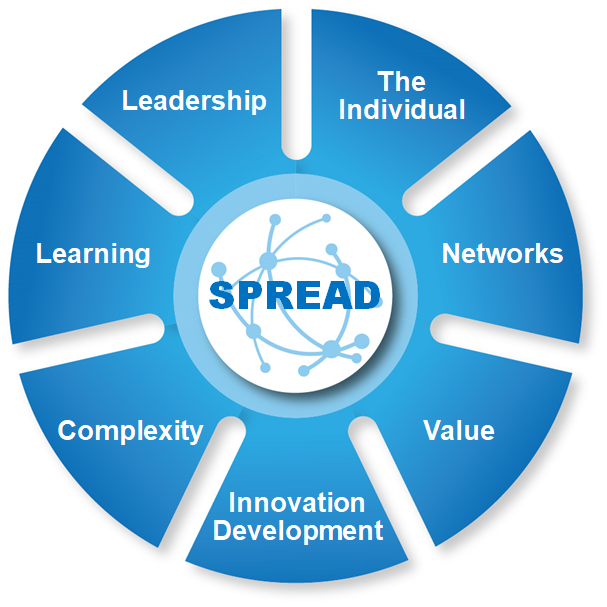
The seven spread and adoption principles [details here]
In the video, Claire describes the challenges of working with complexity and emergence when developing the falls framework as it crosses many organisational boundaries. The importance of bringing difficult conversations back to the individual patient and the shared purpose and shared focus was explained to be crucial to progress and success. Claire describes the importance of remembering value and considering it for the individual patient and also for the whole system e.g. an earlier intervention can avoid a deteriorating patient who may then need hospital admission, so offers value for the individual patient and for the whole system. Continual learning, including through plan-do-study-act (PDSA), is essential. Claire says this is still ongoing and "will never stop" due to the complexity and continual evolving context.
The Falls Framework and Systems Convening
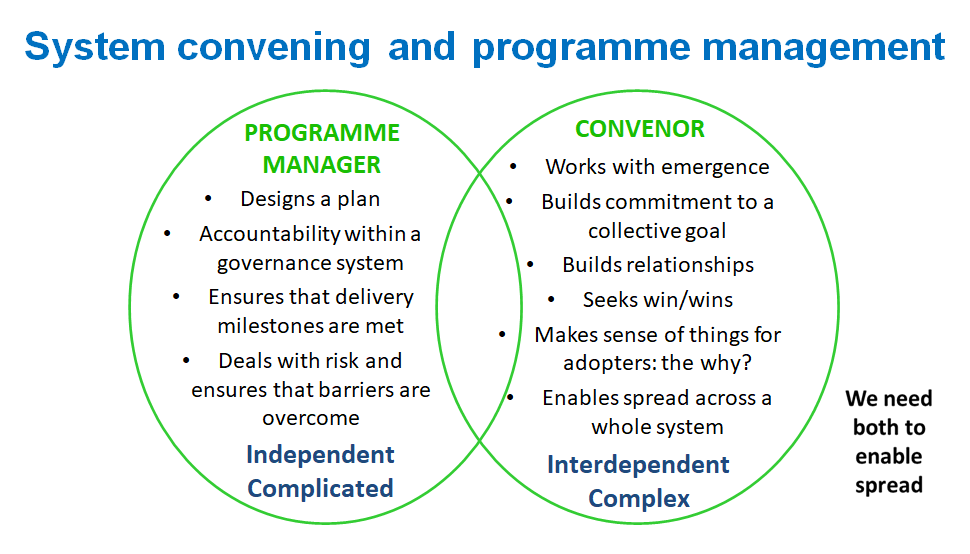
When Claire first saw this graphic she had a ‘lightbulb moment’ and said “I absolutely wish had had the programme management and systems convening slide two years ago. It would have been reassuring to know that it is OK to feel uncomfortable’" while dealing with complexity and emergence.
The falls framework work evolved by people coming together to talk about it, through convening across the system. ‘"As we were doing it I did not think about the theoretical insights’" Claire tells Ian.
An emergent way of working requires emotionally intelligent leadership as it can make people feel uncomfortable. This means you must be able to take people with you on that journey. "We had to try things and take risks which requires emotionally intelligent leadership to do that and to take people with you’"
Claire shares that working with multiple partners felt uncomfortable, as did allowing for emergence rather than having a fixed solution or standard way of working.
There were many times at the beginning of the framework development that Claire felt uncomfortable because thinking about the risks they were taking threw her out of her comfort zone. That discomfort still continues, during many conversations, on a weekly basis.
The interest and comfort in working with emergence to convene across a system can vary between leaders. Claire explains that within the group working together on this falls framework there were various different appetites for moving away from a project management type style to a more emergent style.
For Wales, the falls frameworks is now the ’way we do things’ and work continues to enable to spread, adoption and scale up with local flexibility of implementation to allow for local variation of context e.g. provision of level 1 service.
Further information and reading
- The WAST falls framework was supported by #ProjectA and the Association of Ambulance Chief Executives (AACE) and now forms the basis of national falls guidance for ambulance services. More details can be found through AACE WAST Falls Pathway and Falls Initiative.
- The WAST falls framework was presented at Expo 2019, which you can read about here.
- Enabling leadership requires a mindset shift such that ‘my role is to think about how I can facilitate and enable adaptation, emergence and change’, rather than directing people what to do. Further reading and details on Enabling Leadership here.
- If you're interested in how to enable the spread and adoption of innovations in healthcare, there are previous blogs and further blogs to follow. Please do subscribe to this blog and follow @DianeKetley @HorizonsNHS, #nhsspread.
- Details of NHS Horizons' work on spread and adoption of innovation including the forthcoming online publication is outlined here. We identify the need for a new mindset with an increased understanding of complexity and interdependencies, the need to create a pull of innovation alongside the traditional push approach with attention to relationships and the impact of asking people to change their routines and behaviour.
Image by Senjin Pojskić from Pixabay


/Passle/5a5c5fb12a1ea2042466f05f/MediaLibrary/Images/6168334917af5b10f4bf1d30/2022-04-14-15-27-52-040-62583d78f636e9115805b2d5.png)
/Passle/5a5c5fb12a1ea2042466f05f/MediaLibrary/Images/6168334917af5b10f4bf1d30/2022-08-05-09-59-36-465-62ecea08f636e906acfed639.jpg)
/Passle/5a5c5fb12a1ea2042466f05f/MediaLibrary/Images/6168334917af5b10f4bf1d30/2022-07-28-14-57-17-405-62e2a3cdf636e9180c9835cb.png)
/Passle/5a5c5fb12a1ea2042466f05f/MediaLibrary/Images/6168334917af5b10f4bf1d30/2022-07-20-10-16-56-533-62d7d618f636ea07987f6668.png)
/Passle/5a5c5fb12a1ea2042466f05f/MediaLibrary/Images/6168334917af5b10f4bf1d30/2022-07-15-09-55-32-858-62d13994f636ea1398e71aa9.jpg)